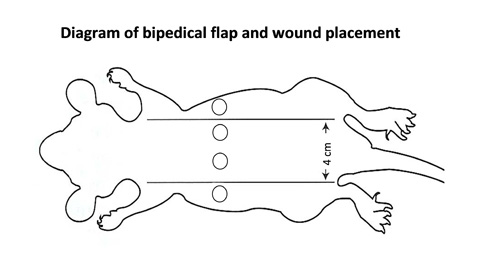
Rat Ischemic Wound Healing
Model Utility:
The rat ischemic wound model is based upon work by Dr. Lisa Gould. The model is designed to mimic wound ischemia by reducing blood flow to wounds through the creation of a bipedical flap on the rodents' back. Once the flap has been created, two, 8mm wounds are created on the back inside the perimeter of the flap. Two additional 8mm wounds are then created outside the flap on the sides of the rat. Without intervention, the ischemic flap wounds heal considerably more slowly than the non-ischemic wounds.
How the model works:
Example data:
The graphs below show two sets of data from a control experiment. In both cases, the wounds inside the flap (labeled B&C) and the wounds outside the flap (labeled A & D) received no treatment other than moist dressing.
In Figure 1, we show the rate of closure of the wounds over time, with the non-ischemic wounds outside the flap closing much faster than the wounds inside the flap.
Figure 2 is an alternative way to represent the data. In this figure, we only count the wounds that have achieved complete closure (total re-epithelialization). So, for example, if 6 out of 10 wounds are completely closed, then the graph will show 60%. Looking at the data this way further underscores the extraordinary delay in healing, with zero of the ischemic flap wounds achieving complete re-epithelialization even after 17 days of healing.
Rodent wounds heal principally by contraction, as opposed to re-epithelialization. This is why the FDA typically requires healing studies to be done in pig models where the skin heals by re-epithelialization as human wounds do. This wound contraction, and the fact that this model is relatively labor intensive (and therefore costly) are the two primary disadvantages to using it as a preclinical screening model.
On the other hand, the model has several advantages as well. In the first place, the delay in ischemic healing is extreme, particularly compared to other acute wound models including pig wounds. This delay enhances the opportunity for active products to demonstrate their efficacy. Secondly, the model is much easier to use than the rabbit ischemic ear model, where even the most experienced laboratories often struggle with replicating published literature. Finally, the use of a rodent species makes it easier to perform secondary assays, such as PK/PD and other safety tests, compared to the larger animal models of wound healing.